Research Group "Virtual Reality Simulation in Medical Education"
Young physicians often lack readily available practical knowledge, as well as the ability to prioritize tasks and make quick clinical decisions during their first years of professional practice. However, these competencies are particularly crucial in emergency situations. Virtual Reality (VR) technology enables the creation of realistic learning environments, allowing students to train in a safe setting with standardized cases. At Universitätsklinikum Würzburg, the VR-based emergency simulation STEP-VR (Simulation-based Training of Emergencies for Physicians using Virtual Reality) was developed in collaboration with the 3D visualization company ThreeDee (Munich). Currently, we are investigating the conditions for the successful implementation of the VR training program in medical education. |
Research topics
Acceptance and Learning Outcomes of VR Simulation
Since 2020, medical students in their 10th semester have been using the VR training program as part of a curricular seminar accompanying their internal medicine clerkship at a teaching hospital. Following the simulation of virtual patient cases, students participate in structured case discussions with instructors. Within an evaluation study, perceived realism (immersion), potential side effects (simulation sickness and stress), and subjective learning outcomes were assessed. The findings indicate a high level of acceptance of VR-based simulation within the seminar format, along with strong perceived learning gains, moderate stress levels, and negligible simulation sickness.
In a subsequent randomized controlled trial, objective competence gains, their long-term retention, and potential influencing factors (e.g., experienced stress during simulation) were examined. The results suggest that VR learning environments can lead to more sustainable knowledge acquisition compared to traditional teaching methods. This study was supported by the Teaching Research Award 2022 of the Vogel Foundation Dr. Eckernkamp.
Feasibility, Fairness, and Validity of VR-Based Assessments
The use of VR in standardized practical examinations such as Objective Structured Clinical Examinations (OSCEs) aims to overcome limitations of conventional assessment formats, including high personnel and material costs, organizational complexity, and limited scenario realism. Funded by the Foundation for Innovation in Higher Education, the existing VR training program was expanded within the VR-OSCE project (2022–2025) to include an examination interface. The results demonstrate that VR-based assessments are technically feasible and can achieve at least comparable psychometric quality to traditional formats.
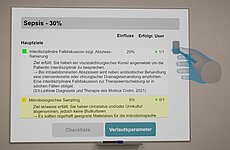
A further study conducted in 2024 used VR simulation to assess the practical skills of early-career resident physicians in managing emergency scenarios. Their objectively measured performance was compared with self-assessments, providing a differentiated picture of clinical competencies: while basic stabilizing measures were generally well performed, deficits were observed in specialty-specific diagnostics and treatment.
Ongoing follow-up studies investigate whether prior experience with VR environments and the ability to operate VR hardware and software (“immersive competence”) influence performance in VR-based assessments. This line of research aims to ensure fairness and prevent disadvantage in future examination settings. In collaboration with the Chair of Human-Computer Interaction at the University of Würzburg, an application for measuring general immersive competence has been developed and tested in a pilot study. Given that current VR systems employ diverse interaction mechanisms, we have also developed an approach to assess immersive competence directly within the application (“in situ”). A recent randomized controlled trial demonstrated a causal relationship between immersive competence and medical performance, highlighting the need for measures to ensure fairness and validity in VR-based assessments.
Development and Evaluation of Interprofessional Multi-User VR Scenarios
In emergency medicine in particular, patient outcomes depend heavily on effective interprofessional collaboration. This subproject aims to extend the VR program with a multi-user functionality, enabling medical students and nursing trainees to jointly manage emergency scenarios in a shared virtual environment. The project was supported and facilitated by WueDive. Since summer 2024, the multi-user functionality has been available, and current research focuses on whether VR environments can effectively support the training of interprofessional teamwork. The training and evaluation are based on the TeamSTEPPS framework, with advisory support from the DACH steering group. Following a pilot phase, the study protocol will be implemented at five additional German sites in early 2025. The Team Performance Observation Tool (TPOT), an established instrument for objective teamwork assessment, has been adapted and validated under our leadership for VR-based scenarios involving interprofessional dyads.
Use of Large Language Models as Virtual Tutors in VR Environments
The project Speaking VirtuAI (Freiraum funding line 2023), funded by the Foundation for Innovation in Higher Education, aims to extend the existing VR learning environment by integrating an AI-based virtual tutor capable of natural language interaction. The project is conducted in collaboration with the Chair for Natural Language Processing (Prof. Goran Glavaš) at the University of Würzburg. This approach is expected to enable a more immersive and individualized learning experience that better accommodates learners’ pace. In addition, it may allow VR-based emergency training to be conducted more frequently and with reduced dependence on teaching staff. Accompanying research investigates whether learning outcomes achieved through AI-based dialogic feedback differ from those obtained through static feedback.
Example images of the appearance and use of the VR environment
Team
- Dr. med. Tobias Mühling (Head of research group)
- Prof. Dr. Sarah König (Head of department)
- Franca Keicher (MD)
- Marco Lindner (MD student)
- Isabelle Späth (MD student)
- Verena Schreiner (MD student)
- Marie Lehmann (MD student)
- Jan Schaal (MD student)
- Alexander Zamzow (MD)
Cooperation partners
- OrangeWhip Interactive - Agency for interactive 3D-visualization (co-developer of STEP.VR)
- Chair for Human-Computer Interaction of Wuerzburg University (News | Human-Computer Interaction (uni-wuerzburg.de))
- Chair for Natural Language Processing of Wuerzburg University (Natural Language Processing)
- Institute of Education and Student Afairs, University of Münster (IfAS)
- Non-Profit Vogel-Foundation Dr. Eckernkamp Würzburg (Home - Vogel Stiftung Dr. Eckernkamp)
Awards and press coverage (German)
- "Virtual Reality im Medizinstudium" in der Wissenslandkarte des bayerischen Instituts für digitale Transformation.
- DGVS Innovationspreis „Digitale Gastroenterologie“ 2019
- Hans-Werner-Feder-Preis der DGINA 2021
- Demonstration beim Besuch des bayerischen Ministerpräsidenten Markus Söder (Artikel in der Main-Post)
- Forschungsförderpreis der Vogel Stiftung Dr. Eckernkamp 2022 (Artikel in der Main-Post)
- eHealth-Podcast Folge #156 – Virtuelle Realität in medizinischer Lehre (Folge #156 - Virtuelle Realität in medizinischer Lehre - eHealth-Podcast)
- Artikel im "Tagesspiegel Background" zum Einsatz von VR in der medizinischen Ausbildung (Notwendigkeit oder spielerischer Gimmick - Tagesspiegel Background)
- Bericht über die erstmalige Durchführung einer VR-basierten OSCE-Station im Medizinstudium (https://www.uni-wuerzburg.de/aktuelles/einblick/single/news/eine-virtuelle-patientin/)
- Podcast „Arbeit Bildung Zukunft“ – Folge #10 „Virtuelle Realität in der Medizinlehre (https://www.wueconomics.de/episodes/abz-02-10-vr-in-der-medizin-lehre)
Publications
- T. Mühling, S. König (2026) Before we trust the scores: rethinking virtual reality in medical assessment. Academic Medicine. https://doi.org/10.1093/acamed/wvag171
- J. Schaal, T. Leutritz, M. Lindner, J. Backhaus, S. König, T. Mühling (2026) Immersive competence as a source of bias in virtual reality clinical assessment. npj Digital Medicine. https://doi.org/10.1038/s41746-026-02482-z
- M. Lehmann, S. Hinz, A. Zamzow, J. Mikulasch, H. Poimann, J. Backhaus, M. Mergen, T. Mühling. Adapting the TeamSTEPPS team performance observation tool for dyadic interprofessional VR simulations (vTPOT): a multi-step validation study. Advances in Simulation (2026). https://doi.org/10.1186/s41077-026-00431-0
- V. Schreiner, J. Backhaus, M. Lindner, M. Heinisch, S. König, S. Oberdörfer, T. Mühling (2026). Specific Immersive Competence in VR-Based Assessments: Development, Psychometric Evaluation and Associations with Medical Performance. JMIR Medical Education. doi: 10.2196/82136
- S. Oberdörfer, M. Heinisch, T. Mühling, V. Schreiner, S. König, M. Latoschik (2025). Ready for VR? Assessing VR competence and exploring the role of human abilities and characteristics. Frontiers in Virtual Reality. https://doi.org/10.3389/frvir.2025.1608593
- F. Keicher, M. Müller, K. Ruf, C. Härtel, S. König, T. Mühling (2025). Enhancing Pediatric Emergency Training: The Impact of Virtual Reality- Simulations on Medical Student Knowledge and Learning Experience. Virtual Reality. https://doi.org/10.1007/s10055-025-01243-9
- T. Mühling, L. Demmler, J. Backhaus, S. König (2025). How Personality and Affective Responses are Associated with Skepticism towards Virtual Reality in Medical Training – A Pre-Post Intervention Study. Cyberpsychology, Behavior, and Social Networking. https://www.liebertpub.com/doi/10.1089/cyber.2024.0567
- M. Lehmann, J. Mikulasch, H. Poimann, J. Backhaus, S. König, T. Mühling (2025). Training and Assessing Teamwork in Interprofessional Virtual Reality-based Simulation using the TeamSTEPPS framework – Protocol for a Randomized Pre-post Intervention Study. JMIR Research Protocols https://www.researchprotocols.org/2025/1/e68705
- M. Lindner, T. Leutritz, J. Backhaus, S. König, T. Mühling (2025). Knowledge Gain and the Impact of Stress in a Virtual Reality-based Medical Emergencies Training with Automated Feedback – A Randomized Controlled Trial. Journal of Medical Internet Research https://www.jmir.org/2025/1/e67412
- T. Mühling, V. Schreiner, M. Appel, T. Leutritz, S. König (2025). Clinical Competency Assessments: A Comparative Study of Virtual-Reality-Based and Traditional Physical OSCE Stations. Journal of Medical Internet Research https://www.jmir.org/2025/1/e55066
- F. Keicher, J. Backhaus, S. König, T. Mühling (2024). Virtual reality for assessing emergency medical competencies in junior doctors – a pilot study. International Journal of Emergency Medicine. https://doi.org/10.1186/s12245-024-00721-2
- M. Lindner, T. Leutritz, J. Backhaus, S. König, T. Mühling (2023). Kompetenzgewinn und der Einfluss von Stress in einer Virtual Reality-basierten Notaufnahme. Jahrestagung der Gesellschaft für Medizinische Ausbildung 2023. doi: 10.3205/23gma151
- F. Keicher, T. Mühling, M. Müller, K. Ruf, S. König (2023). Von der Theorie in die (simulierte) Praxis – pädiatrische Notfälle in Virtual Reality für PJ-Studierende und BlockpraktikantInnen. Jahrestagung der Gesellschaft für Medizinische Ausbildung 2023. doi: 10.3205/23gma177
- T. Mühling, I. Späth, J. Backhaus, N. Milke, S. Oberdörfer, A. Meining, M. Latoschik, S. König (2023). Virtual reality in medical emergencies training: benefits, perceived stress, and learning success. Multimedia Systems. DOI: https://doi.org/10.1007/s00530-023-01102-0
Contact us
For inquiries, please contact: Tobias Mühling , MD (muehling_t(at)ukw.de)